
I’m extremely flattered by being the individual chosen to receive this year’s MMRF Spirit of Hope Award for the Twin Cities 5K Walk/Run fundraising event. But unfortunately, it’s also partly the result of being a multiple myeloma patient, which means I have a cancer that currently does not have a cure. And that is by far the number one reason I’m passionate about doing my part to help find a cure for this disease. But it’s not just about me—it’s about all the other myeloma patients and caregivers I read about, listen to through Patient Webinars, and see at Lake Phalen every year doing everything they can to help find a cure for us patients, so we and future myeloma patients can live a full life with all those individuals who love us so much.
A few other organizations are out there that are also working to find a cure for myeloma. So that begs the question: Why did I choose the MMRF as the organization I wanted to put my time and energy behind? To determine that, I asked myself a pretty simple question: What is the best possible way to find a cure for myeloma? I believe the answer is through research. When I looked at the track record of the various organizations, two stood out to me because of the number of years they’ve been in existence, and they both were started by individuals who were directly impacted by myeloma. Two criteria separate the MMRF from all the others: over 90% of the funds it raises go directly toward research, and it has a major fundraising event right in my backyard. Bingo! We have a winner! Just look at the amount of money the MMRF has given to date toward research, over $600 million! Yes, over $600 million dedicated directly to finding a cure for myeloma. All of us need to do our part in helping to generate more funding for research, so we have a chance to win our fight to live and realize the love of all our family members and friends who have been there for us because they want us to live.
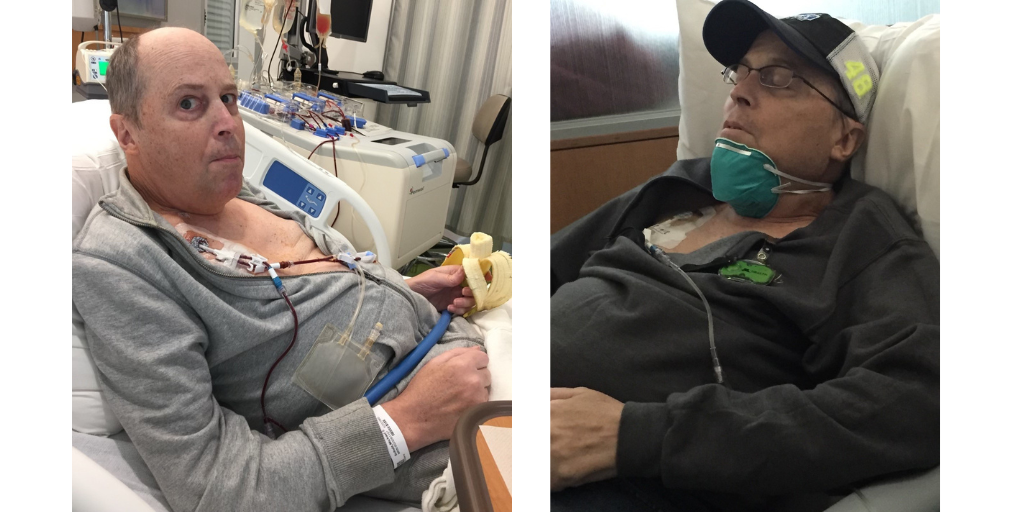
What I admire the most are those family members and friends that have continued to help raise money for research, in spite of the fact that their loved ones that they fought for fell short of winning their battles. These are the ones who most emulate what the Spirit of Hope stands for, and they are the true winners of this award. Last year, four teams raised over $10,000 for the Twin Cities 5K Walk/Run fundraising event. My team was one of them, and we brought in the lowest total of the four teams. But get this, the other three teams raised their donations in remembrance of loved ones who used to stand with us Living Proof members in years gone by now, but the teams continue to act because of what those people meant to them and don’t want our caregivers to have the same results as they did.

HOPE. It’s a word that carries a heavy load. It’s also a word that I believe in. I do have hope. When I was first diagnosed back on January 17, 2012, I was told I would be lucky to live a year and a half. I’ve relapsed two times and have participated in two clinical trials. Twelve and a half years later, I’m still here. Why? I have a lot of faith and believe that God wants me to still be here for a reason that only He knows. In addition, since I was first diagnosed, eleven new forms of treatment have been approved by the FDA, I’m currently on one of them (daratumumab or Darzalex) for maintenance. A whole new field of treatments is coming on the scene and is starting to explode with different variations. I’m talking about immunotherapy, which includes CAR-T therapy and bi-specific therapies. The results are extremely promising. And that means HOPE—hope that someday soon, we’ll yes, we’ll find a cure. Join me and my team, The Mike Schulz Marchers, at this year’s Twin Cities 5K Walk/Run Fundraising event. Let’s give the Living Proof photo a whole new meaning.
Sincerely,
Mike Schulz
The MMRF is delighted to recognize Mike Schulz as the MMRF Spirit of Hope Honoree at the 2024 MMRF Team for Cures: Twin Cities Walk/Run. Donate to his fundraising page to accelerate a cure today!
This award is presented at every Walk/Run to a patient, caregiver, or family who inspires hope through their resilience, perseverance, and dedication to the MMRF and its mission.